
Healthy Knee Physiotherapy Program
1 on 1 Physiotherapy for your Knees
Calgary Core Physio will work with you to increase your knee function, and reduce knee pain.
At Calgary Core Physiotherapy, we love helping patients with their knee injuries. Whether it is an acute knee injury, knee pain that you have been struggling with for years, or following knee surgery, our physiotherapists have years of extensive experience working with knees. The Calgary Core Physio Healthy Knee Program involves attentive, efficient, and individualized care for your knee problem.
What does our Healthy Knee Program include?
-
Assessment
A thorough assessment of your knee by an experienced physiotherapist that focuses on achieving a diagnosis of your problem, as well as contributing factors to help realize the big picture.
-
Ongoing Evaluation
Movement evaluation, how your muscles are working or not working, what your other joints look like and figuring out the “core” issues of your pain and injury.
-
Imaging (if needed)
Appropriate referral for diagnostic imaging, such as an x-ray or MRI, if required
-
An action plan
Based on years of clinical experience and the most current research, a treatment plan to improve pain and function
-
A treatment schedule
Prompt and effective treatment by team members at the clinic with the focus of getting you better, faster
-
Physician/Health Care consult (if needed)
Working closely with your family physician and other health care providers and, if necessary, “quarterbacking” your treatment plan
-
Fitness rehab recommendations
Communication with coaches, personal trainers or other providers to review and manage optimal activity level and exercises for your knee.
What are the typical conditions that this program can help with?
The most common conditions that the Calgary Core Physio Healthy Knee Program addresses are:
The iliotibial band (ITB) is a large fibrous band of fascia and connective tissue that runs from the pelvis (ililum) to the shin bone (tibia). The ITB is important for the stability of the knee and leg. The bottom end of the ITB moves forward and backward as the knee bends and straightens. A painful condition can sometimes occur due to repetitive rubbing and resultant friction at the side of the knee. This pattern is the primary source of pain and injury to the outside of the knee.
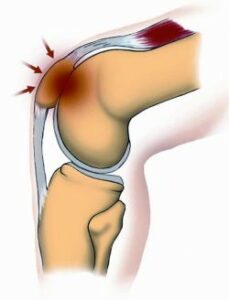 Patellofemoral Pain Syndrome is a painful condition involving the front aspect of the knee. It involves pain or irritation behind the kneecap (patella) due to excessive compression where the kneecap contacts the thigh bone. This may occur due to poor tracking of the kneecap or muscular imbalances around the kneecap. Risk factors include muscle weaknesses, tight knee structures, over-training, and previous injuries to the hip, knee or ankle. Pain is normally worse after activity, going up or down stairs and after keeping the knee bent for prolonged periods, such as with sitting.
Patellofemoral Pain Syndrome is a painful condition involving the front aspect of the knee. It involves pain or irritation behind the kneecap (patella) due to excessive compression where the kneecap contacts the thigh bone. This may occur due to poor tracking of the kneecap or muscular imbalances around the kneecap. Risk factors include muscle weaknesses, tight knee structures, over-training, and previous injuries to the hip, knee or ankle. Pain is normally worse after activity, going up or down stairs and after keeping the knee bent for prolonged periods, such as with sitting.
The meniscus is the spongy, cartilage material in the knee joint that protects the knee by helping absorb shock and providing extra stability to the knee. There is an inside meniscus (medial) and an outside meniscus (lateral). The meniscus can be torn by a twisting mechanism or excessive bending of the knee. It also can slowly degenerate over time. In more severe cases of a torn meniscus, the knee joint can “lock,” in which it is unable to bend or straighten.
The anterior cruciate ligament (ACL) and the medial collateral ligament (MCL) are the most common ligament injuries in the knee. Both ligaments can be injured on their own or in combination with the other. These ligaments become sprained with a traumatic injury, usually involving a twist and a force towards the inside of the knee. A ligament sprain is graded from 1 to 3, in which a grade 1 sprain involves just a few of the ligament fibers torn, and a grade 3 sprain involves the whole ligament being torn and unstable.
Knee Osteoarthritis is inflammation and a “wearing down” of the knee joint, in which the cartilage that lines the knee joint becomes thinner, the joint space between the thigh (femur) and shin (tibia) reduces, and extra bone called osteophytes may form within the joint. Previous trauma to the knee, increasing age, or being overweight can predispose someone to osteoarthritis in the knee.
Interested? Want to book? Let's talk.
You can call us at (403) 455-4010, or use the form below. We'll reply within 1-business day.
Your lasting recovery is our priority.
Let’s get you better:


