

Physiotherapy Clinic in Downtown Calgary
Our physiotherapists use a treatment approach that combines various therapies, specially tailored for the most effective way to manage your injury.
-
service

-
service
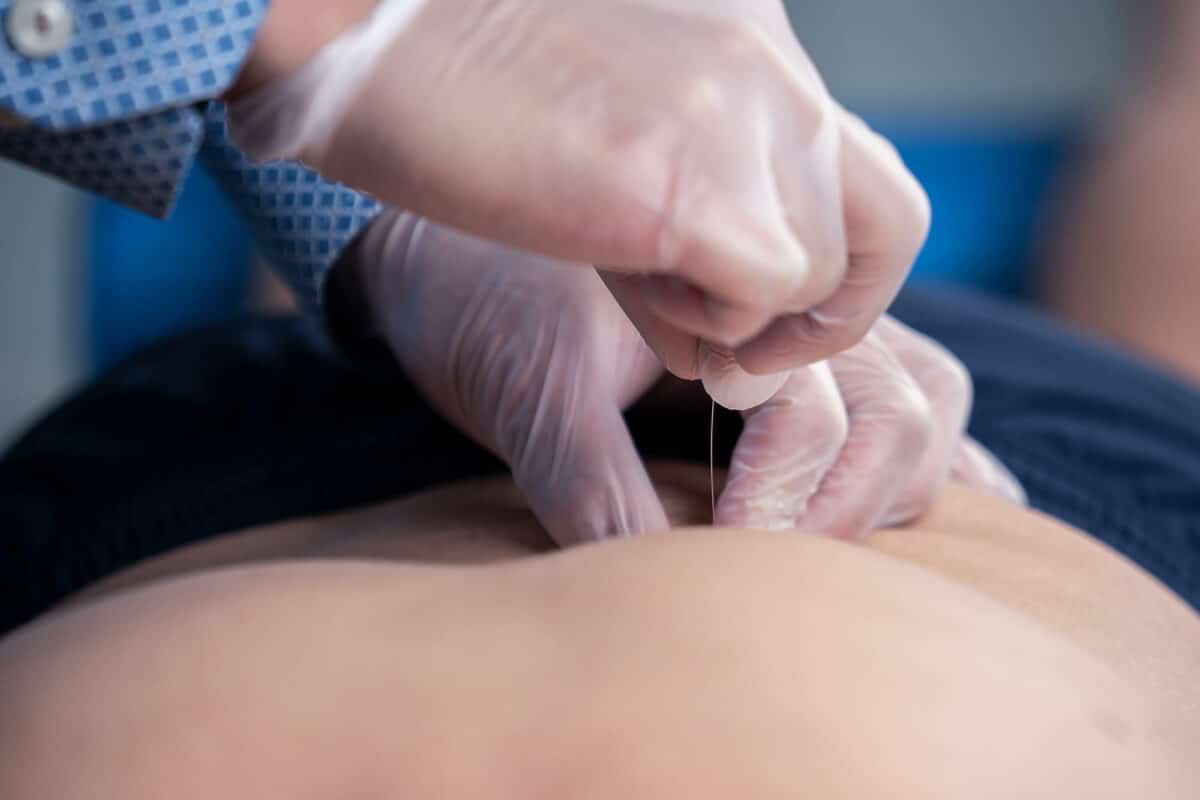
Intramuscular Stimulation (IMS)
-
service
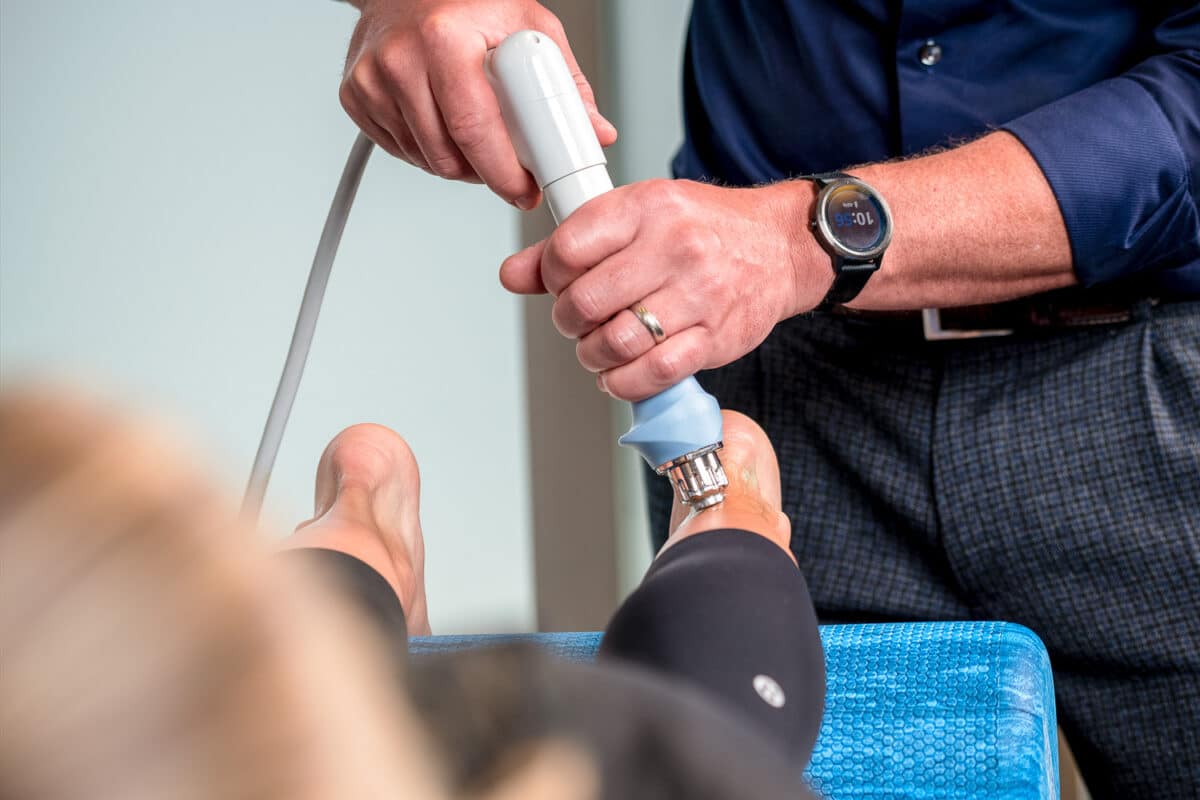
Shockwave Therapy
-
service
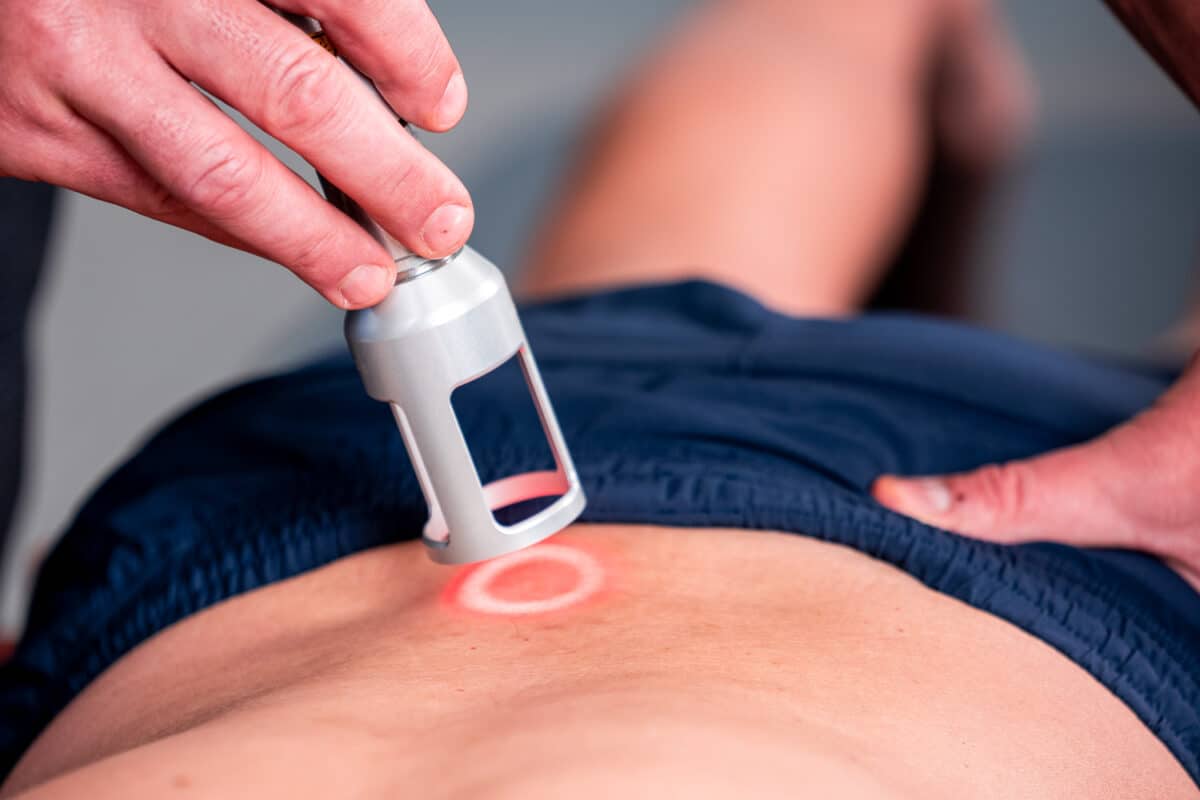
Class IV Laser Therapy
-
service
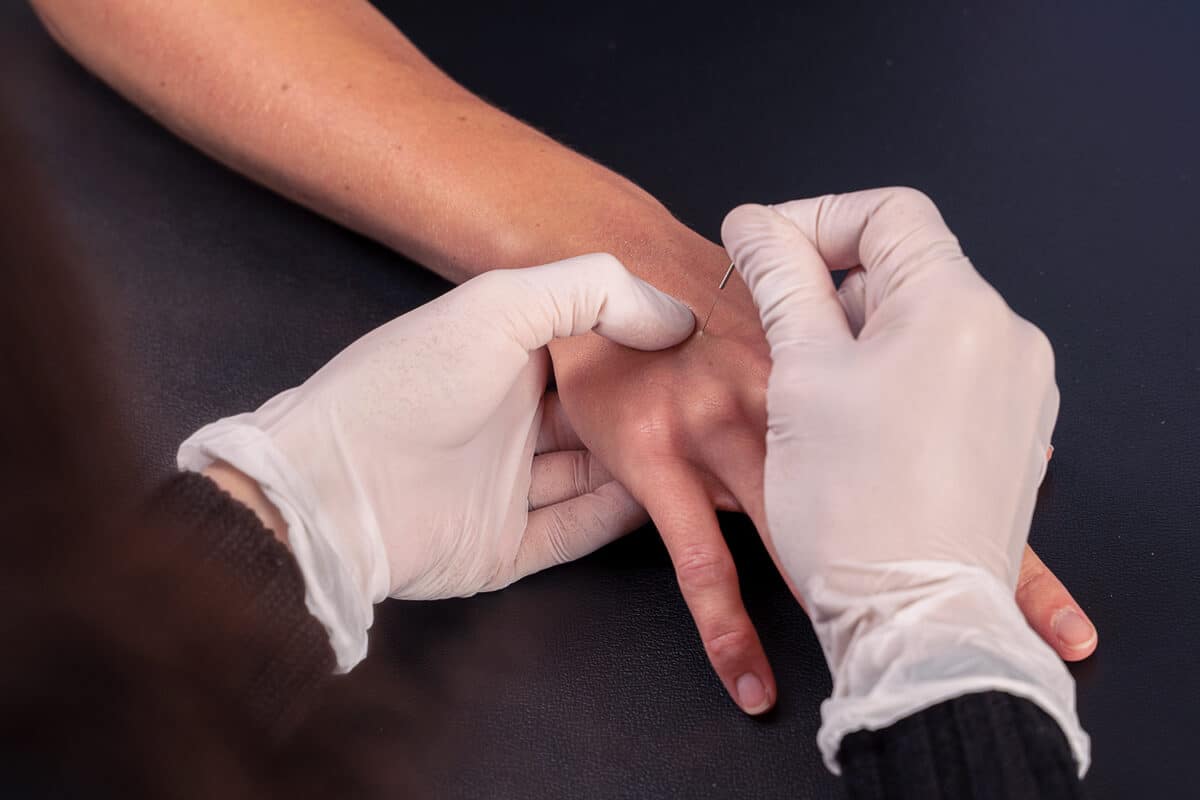
Medical Acupuncture
-
service
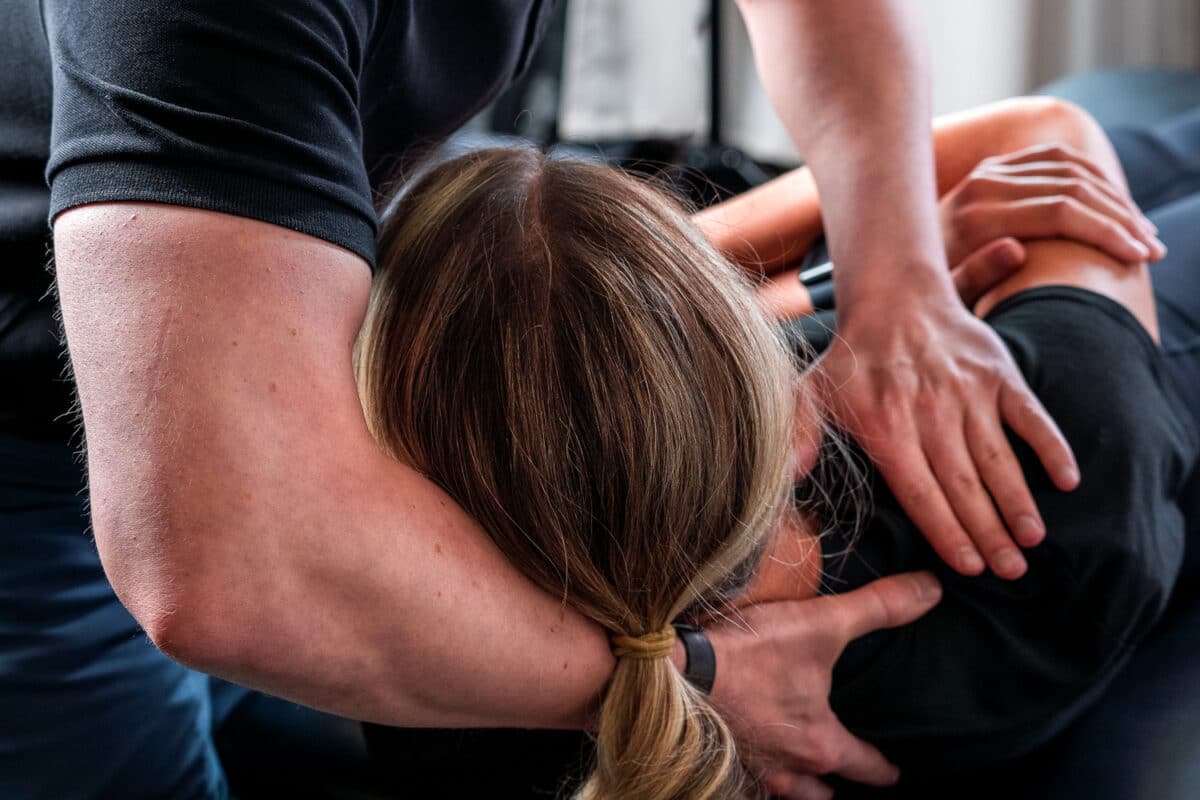
Muscle Activation Techniques (MAT)™
-
service
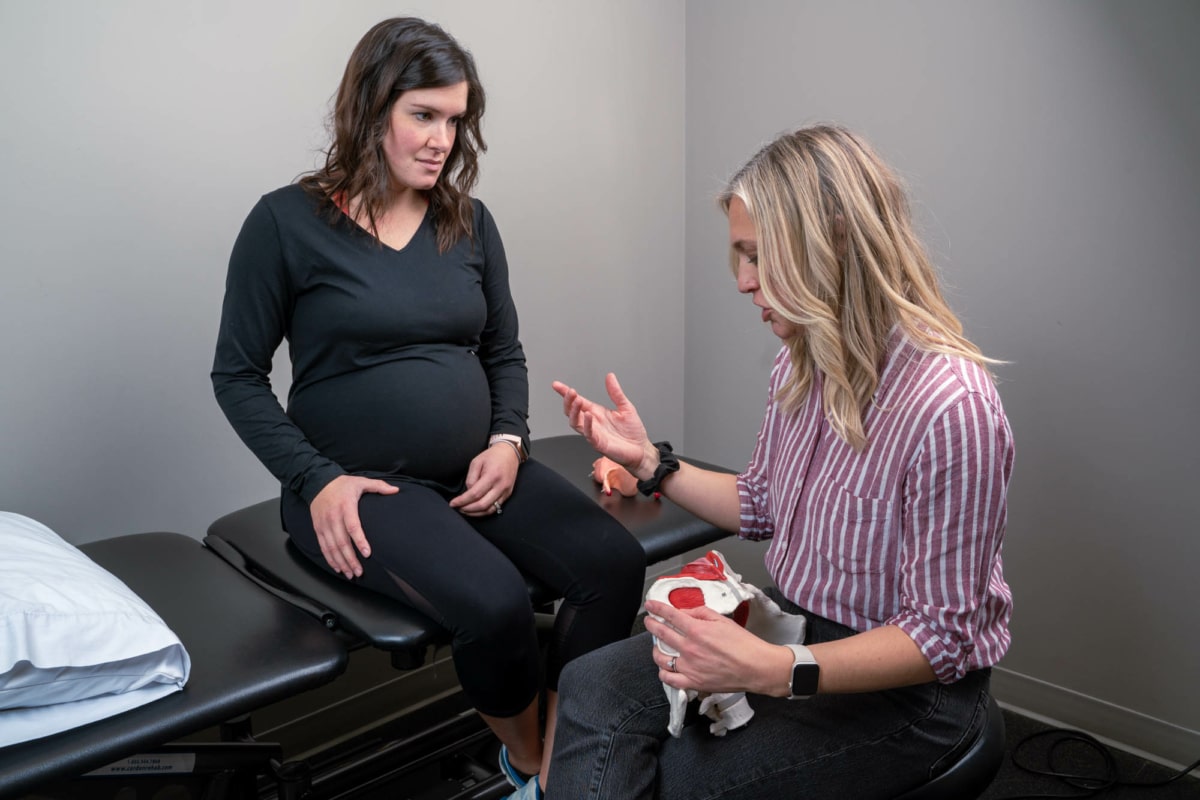
Pelvic Health Physiotherapy
-
service

Massage and Soft Tissue Therapy
-
service
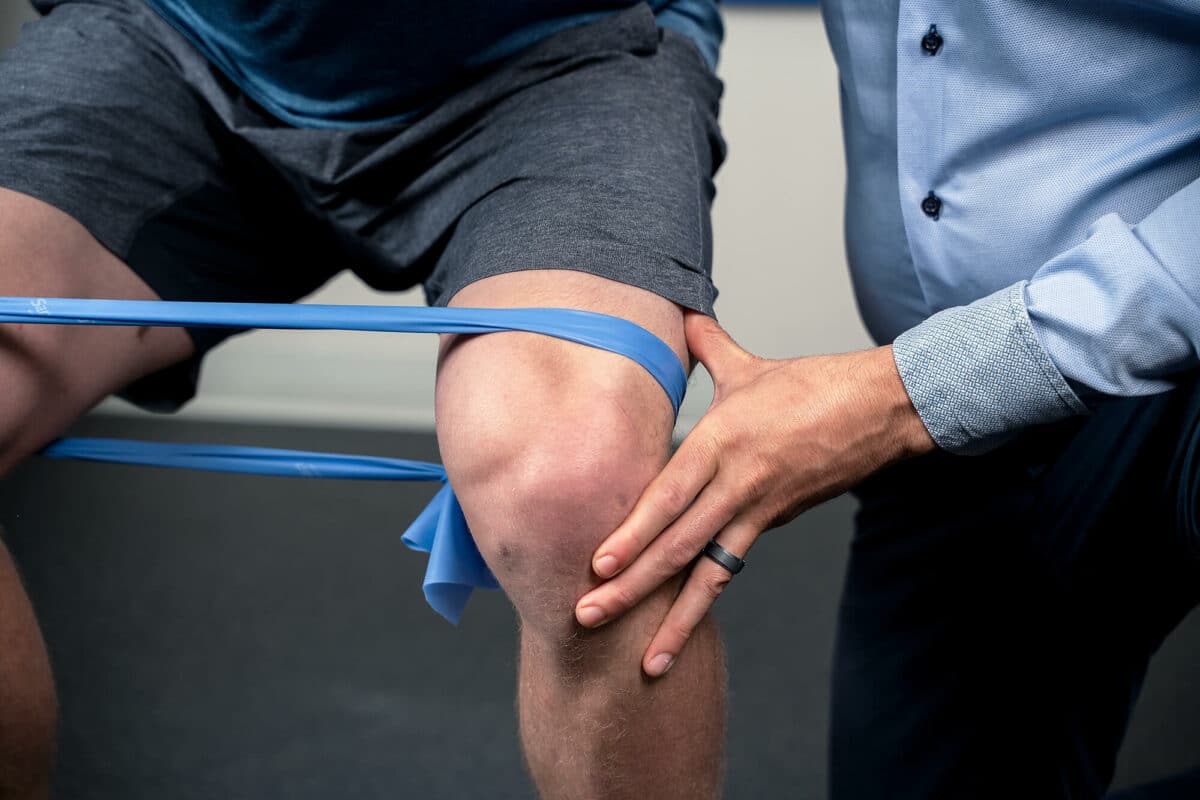
Sport-Specific and Post-Operative Rehabilitation
-
service

Exercise Prescription
-
service
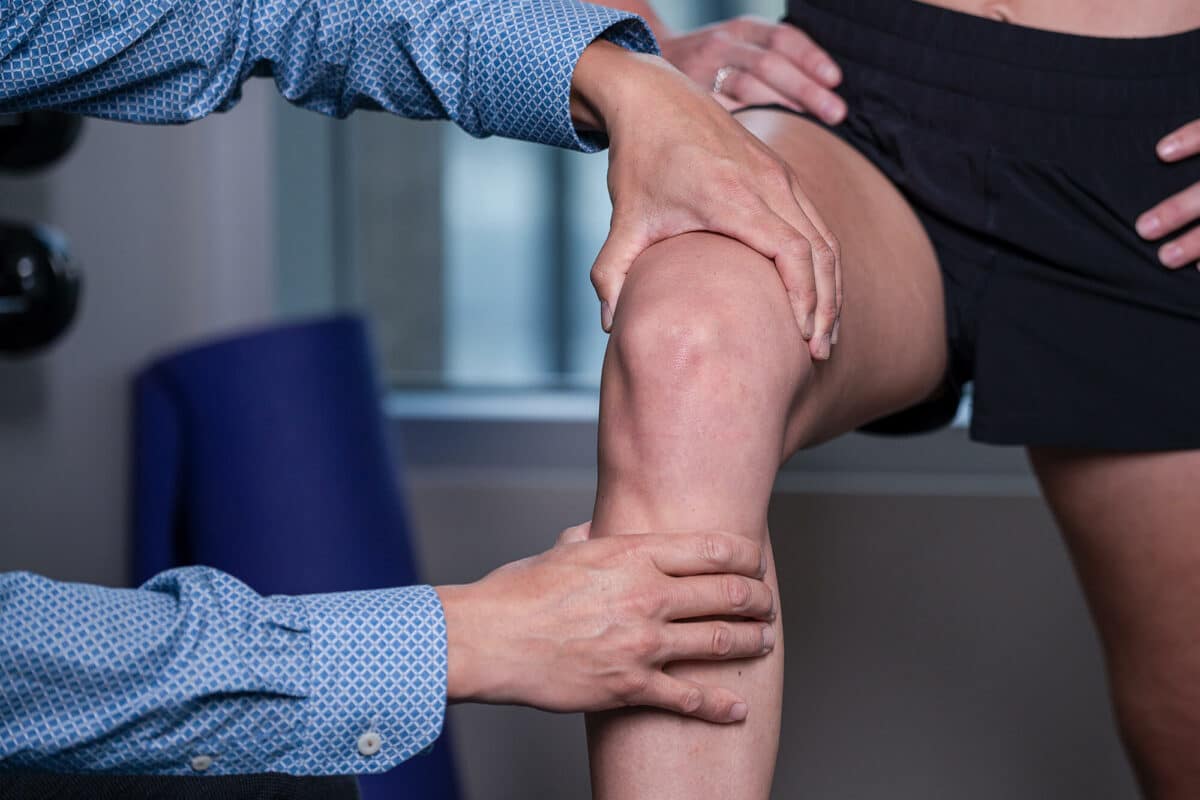
Running Gait Assessment
-
service
X-Ray, Ultrasound, MRI Referral
-
service

Virtual Physiotherapy Consultation
We focus on getting to the Core issues of your injury. Not just putting 'bandaids' on your pain.
Our Physiotherapy Services
Our personalized treatment approach involves:
- Attentively listening to you regarding your pain and problems, and performing a thorough evaluation of your injury
- Gathering all pertinent information and providing you with a diagnosis
- Teaching you about your injury and answering any questions you may have
- Choosing and combining the most effective treatments to help you get better and faster, using our experience and knowledge of up-to-date research
- Communicating with your existing health care team, or when necessary, providing you a referral to our strong network of sports medicine and pain physicians, podiatrists, registered massage therapists, Pilates instructors, yoga instructors, and personal fitness trainers

A quick summary of all our services
Do you have an injury but just don’t have the time to make it into our clinic for treatment? Calgary Core Physiotherapy is now offering custom Online One-on-One Physiotherapy consultations using online video. Call us to find out more about this exciting service!
Joint manipulation involves a quick, but small thrust to a joint (e.g., neck, back, ankle, elbow) to provide immediate pain relief and improved mobility. Joint mobilization is a slower movement of a joint in a specific direction.
IMS involves the careful insertion of acupuncture needles into tight muscle bands or trigger points to stimulate a “twitch” response in the muscle. This stimulation causes a reflex relaxation of the muscle with the goal of alleviating pain, muscle tightness, and improved movement.
Your physiotherapist will carefully analyze any imbalances or deficiencies in your muscles, joints, nerves, and overall movement. We provide you with a customized exercise program to improve your injury condition by addressing your flexibility, strength, stability, balance, coordination, and any sport-specific skills.
Shockwave Therapy is an effective therapy that uses acoustic waves directed at chronically inflamed and painful tissues. It reverses the chronic inflammatory process and accelerates healing of the injured tissues in such conditions as plantar fasciitis, rotator cuff tendonitis, and other tendon injuries.
Class IV Laser Therapy is an advanced, non-invasive laser energy used to accelerate the healing of injured tissues. Supported by laboratory and clinical research, this form of treatment can help alleviate your pain, reduce inflammation, and speed up recovery from a wide range of acute and chronic clinical conditions.
While we are not massage therapists, physiotherapists apply various advanced massage and soft tissue techniques targeting injured tissues to promote healing. At Calgary Core Physiotherapy, we believe in a “hands-on” approach to treatment.
Prolotherapy is a safe, effective, non-surgical treatment involving injections of chronically injured ligaments and tendons provided by a medical professional. Prolotherapy involves the injection of hypertonic dextrose, mixed with a local anesthetic.
Medical Acupuncture is the blending of Traditional Chinese Medicine and Western medicine to treat orthopedic conditions. Your physiotherapist will insert acupuncture needles into acupuncture points that are specifically chosen for your injury to provide you with pain relief and improved healing.
Whether you’re a competitive or recreational athlete, your physiotherapist will work closely with your coaches, training program, or personal goals to get you back on track as soon as possible. If you have undergone surgery, your physiotherapist will provide you with optimal treatment and exercise progression in your rehabilitation.
Muscle Activation Techniques (MAT)™ is an advanced manual therapy technique designed to identify and correct muscular imbalances by improving stability in the muscular system. The fundamental principle of MAT is that muscle tightness is secondary to muscle weakness.
Your physiotherapist will determine if an x-ray, ultrasound, or MRI referral is warranted or necessary for your injury condition.
Referrals are for patients in Calgary, Alberta.
These diagnostic imaging tests can assist in gaining further information to confirm a diagnosis and course of treatment.

Learn about our Physio Rehab Programs
Physiotherapy Rehab ProgramsYour lasting recovery is our priority.
Let’s get you better:


